Medical Billing Audit
Home / Services / Medical Billing Audit
Medical Billing Audit Overview
A medical billing audit is a detailed review of billing practices, coding accuracy, and claim submissions to ensure compliance with payer regulations and industry standards. Our audit process identifies errors, inefficiencies, and revenue leakage that may impact your financial performance. By evaluating documentation, coding patterns, and reimbursement trends, we help healthcare practices improve accuracy, reduce compliance risks, and strengthen overall revenue integrity—creating a more transparent, efficient, and financially secure billing operation.
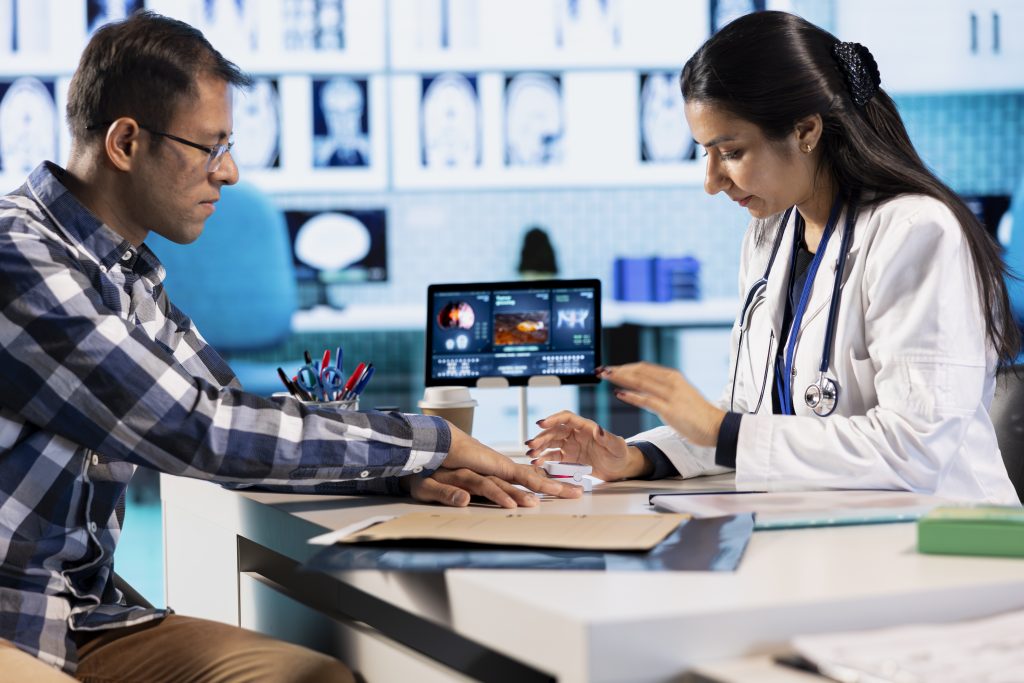
Why Medical Billing Audits Matter
Medical billing audits play a critical role in protecting your practice from financial losses and compliance risks. Even small coding or documentation errors can lead to denied claims, delayed reimbursements, or regulatory penalties. Our audits help uncover hidden issues such as undercoding, overcoding, missed charges, and inconsistent billing practices. By identifying these problems early, practices can improve claim accuracy, enhance compliance, and ensure they are receiving the full reimbursement they are entitled to. Regular audits also strengthen internal processes, reduce future errors, and support long-term financial stability.

Error Detection

Revenue Protection

Compliance Assurance
Reduce audit risks by aligning billing practices with payer and regulatory standards.
Process Improvement
Strengthen internal workflows and prevent repeat errors through actionable insights.

Benefits of Choosing Our Billing Services
Our medical billing audits uncover a wide range of issues that can silently affect revenue, compliance, and operational efficiency. By reviewing claims, coding patterns, and documentation, we identify gaps that often go unnoticed in day-to-day billing processes.
Key issues we identify include:
- Duplicate or incorrectly submitted claims
- Missing or incomplete documentation
- Incorrect modifier usage
- Repeated claim denials and rejections
- Inconsistent billing workflows
- Payer-specific compliance gaps
- Unbilled or missed charges
Our Audit MethodologyOur Audit Methodology
We follow a structured and transparent audit approach designed to deliver accurate insights and measurable results. Our methodology combines detailed data analysis with industry best practices to ensure every aspect of your billing process is reviewed thoroughly. This systematic process allows us to identify risks, uncover revenue opportunities, and provide clear recommendations without disrupting daily operations.
Our audit process includes:
Comprehensive review of claims, coding, and documentation
Evaluation of payer-specific billing rules and compliance standards
Analysis of denial patterns and reimbursement trends
Identification of revenue leakage and process inefficiencies
Detailed findings with prioritized recommendations

